XVIVO is helping Medical History Pictures, Inc. to develop 3D animation for a biographical documentary about Dr. Maurice Hilleman (1919-2005), one of the most important contributors to modern vaccinology. We will routinely update with behind-the-scenes images while providing some science notes and musings.
Vaccines against viruses are said to be made of dead or weakened pathogens, which already hints at the existence of two different types of vaccines. While there are many different strategies used to create vaccines, let’s take a moment clarify this notion of “dead” and “weakened” viruses a bit, and what they really are.
Dead viruses, more accurately known as inactivated viruses, are viruses that have had their virulence destroyed. A few posts ago, we told you that viruses aren’t classified as living, so what does it actually mean to have a “dead virus”? A dead (inactivated) virus is a virus that has had its infective potential removed, either by chemical alterations or extreme heating to the point that it can no longer invade your cells.
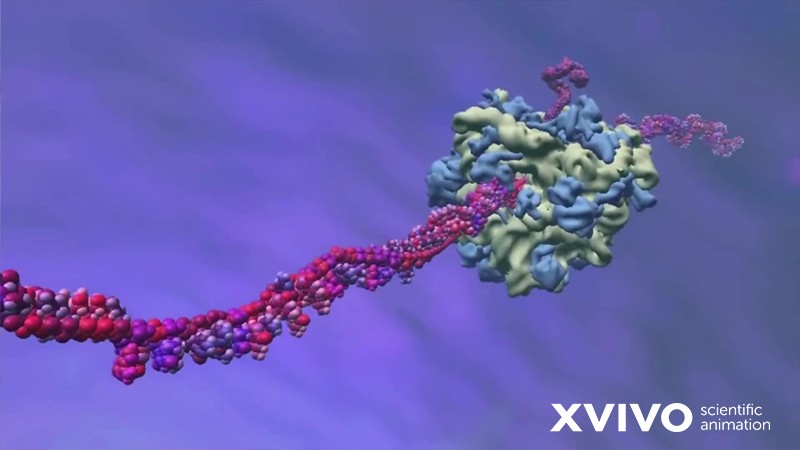
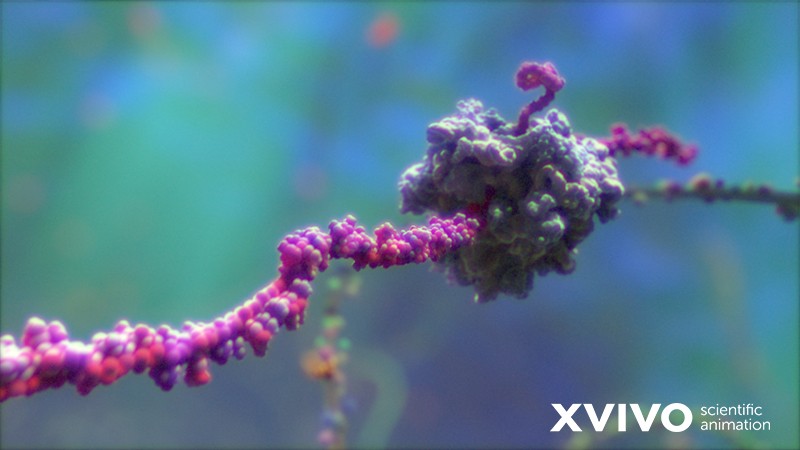
Sounds great, right? Why don’t we just always use dead viruses for our vaccines?
Because viral inactivation results in an alteration of viral protein structure, these “dead” viruses generally don’t protect as well as the “live” ones when used for vaccination. The effectiveness of an inactivated viral vaccine is dependent both on its ability to elicit a strong immune response and the similarity of the “dead” virus to its “live” counterpart. Many of these types of vaccines require boosters to establish long-term immunity.

How do weakened vaccines work? What does it mean to “weaken” something like a virus?
Weakened viruses, or attenuated viruses, are viruses that have been cultured in cells of a different animal. This allows us to select for a mutant variant that is better at infecting non-human cells and less effective at infecting humans. By keeping the virus slightly related to its original form, but not quite as infectious to humans, it can help train our bodies into building a suitable immune defense. Live, attenuated vaccines are made to be as close to a natural infection as possible, and generally provide better and longer-lasting defenses.
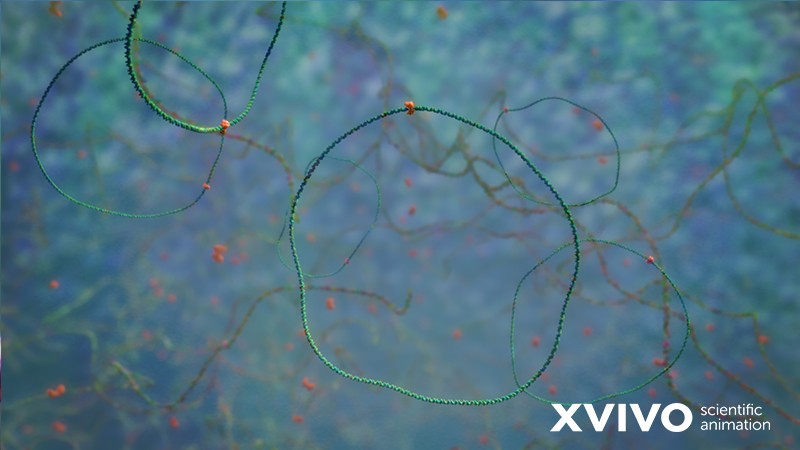
Sounds great, why don’t we just always use live, attenuated vaccines?
They need to be kept “alive”. Live vaccines require refrigeration, making it difficult to store and ship to places where reliable equipment is harder to come by. It’s also harder to make an effective attenuated virus, as new viral generations need to be closely monitored to ensure both safety and maximal effectiveness. Since live viruses can still invade cells, replicate, and mutate, there is also that small chance that they may mutate back to their virulent form. This is known as reversion. While the probability of this happening is very small, it’s still something important to note for both vaccine development and administration.
